Wilmington Health Gastroenterology provides comprehensive care for conditions affecting the digestive system, including the stomach, colon, small intestine, liver, pancreas, and gallbladder. Our experienced team specializes in diagnosing and treating a wide range of digestive disorders—from common concerns like reflux, abdominal pain, and irritable bowel syndrome to more complex conditions such as inflammatory bowel disease and liver disease.
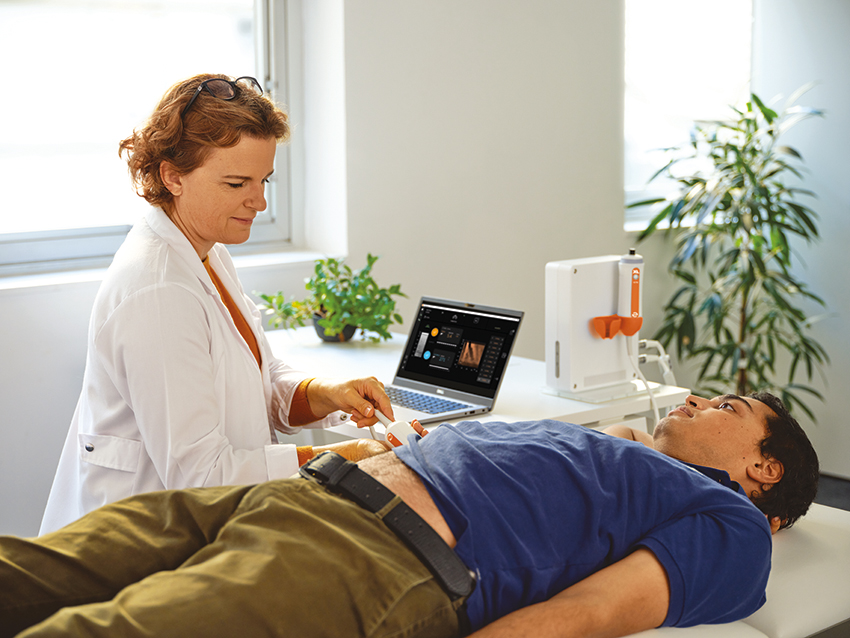
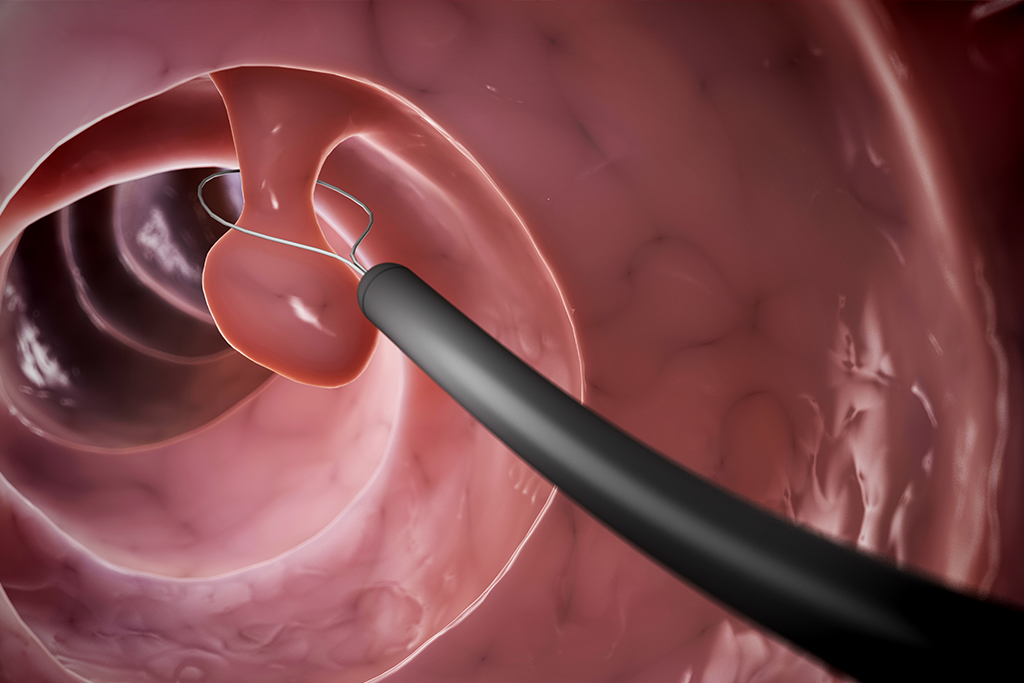
Prevention and early detection are also a vital part of what we do. Our providers perform important screenings such as colonoscopies to help detect colon cancer early, when it is most treatable. We also offer advanced diagnostic technology, including small bowel capsule (pill cam) endoscopy and FibroScan®, a non-invasive, in-office test used to evaluate liver health and detect fibrosis or scarring.
At Wilmington Health, our board-certified gastroenterologists work closely with each patient to create personalized care plans that not only treat digestive conditions, but also help patients maintain long-term digestive health and overall well-being.